When Disaster Becomes the Teacher
A timely lecture by the LAU school of medicine examines how structured emergency preparedness plans strengthen hospital readiness.
In light of alarming developments in the country and the region, on March 10, 2026, the LAU Gilbert and Rose-Marie Chagoury School of Medicine dedicated a session of its Grand Round Series, organized by the Office of Continuing Medical Education and Professional Development, to hospital preparedness in an emergency.
Titled From Planning to Action: Emergency Preparedness in Healthcare and the LAU Medical Center–Rizk Hospital Institutional Experience, the lecture aimed to inform medical teams and hospital leaders on the principles of emergency preparedness planning in healthcare systems and their critical role in ensuring coordinated and effective responses during disasters.
For Lebanon’s hospitals, which must once again face a humanitarian crisis, the discussion carried particular weight. Over the past several years, these institutions have been forced to step up amid successive calamities—from the Beirut port explosion, the pager attacks, to an ongoing economic collapse—each testing their capacity and resilience. While devastating, these events have also generated critical lessons in adapting and strengthening emergency response.
Sessions like this Grand Round Series reflect the school’s commitment to graduating physicians who are not only clinically excellent but also trained to lead when it matters most, noted Dean Sola Aoun Bahous.
“We believe that medical education does not end in the classroom; it is forged in the crucible of real-world crises,” added Dr. Aoun Bahous. “Lebanon’s hospitals have endured extraordinary hardships, and the lessons they carry are among the most valuable we can offer our students and the wider medical community.”
Leading the session was Clinical Associate Professor and Division Head of Emergency Medicine Mariana El Helou, who also serves as a professional mass casualty trainer for European institutions within the World Health Organization (WHO). Having overseen emergency preparedness efforts at the LAU Medical Center–Rizk Hospital, Dr. El Helou demonstrated how hospitals can transform crisis experience into structured, effective preparedness.
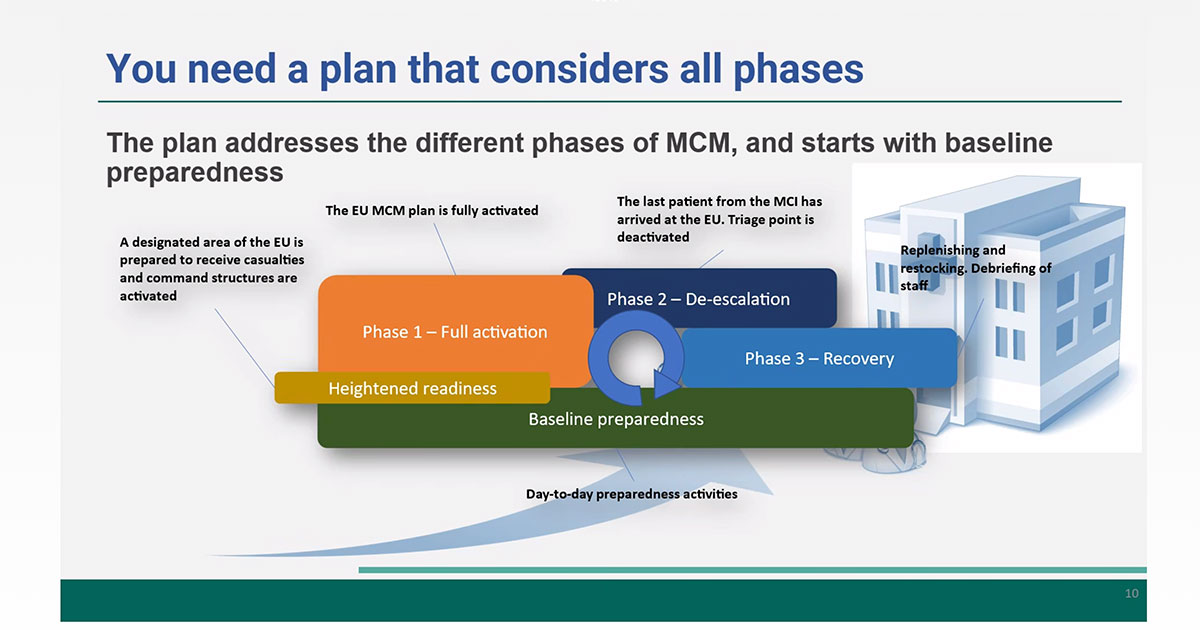
Hospital preparedness, pointed out Dr. El Helou, does not exist in isolation. An Emergency Preparedness Plan (EPP) must function within a coordinated hierarchy that connects emergency departments, healthcare institutions, regional authorities and national systems. Its effectiveness depends on the alignment of these interconnected layers. However, even the most comprehensive plan has limits.
“Mass Casualty Incidents (MCI) are never the same, and no EPP can be created to accommodate all hazards,” noted Dr. El Helou. “EPPs can follow all the major rules, but adaptation and improvisation are needed in an MCI response.”
Drawing on the medical center’s experience, Dr. El Helou described how the hospital’s preparedness framework has evolved in response to real-world emergencies. The Beirut port explosion, which sent thousands of casualties to hospitals across the capital within hours, revealed critical operational challenges—from crowd control and internal communication breakdowns to unclear role assignments during the surge.
“Each disaster, as difficult as it was, became a source of hard-won knowledge that shaped a stronger emergency response framework,” she said.
In the years since, the LAU medical center has implemented a series of structural improvements to strengthen its emergency readiness. It now operates with a clearly mapped emergency department layout, real-time color-coded alert systems shared across staff and trainees and standardized emergency kits that include clinical forms developed by the WHO.
Color-coded vests identify team leaders during response operations, while role-specific action cards outline responsibilities during mass casualty events, helping eliminate uncertainty at critical moments.
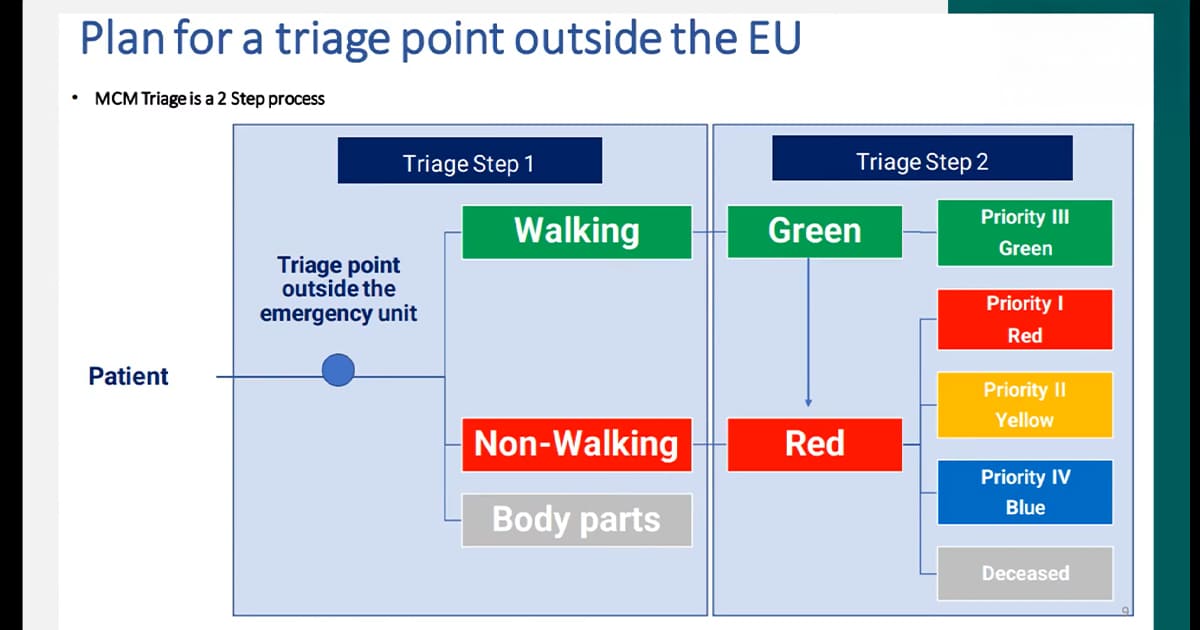 Triage procedures were also revised. In large-scale emergencies, Dr. El Helou explained, the primary objective is rapid prioritization: Identifying the small percentage of patients who require immediate life-saving intervention and ensuring that resources are directed where they can have the greatest impact.
Triage procedures were also revised. In large-scale emergencies, Dr. El Helou explained, the primary objective is rapid prioritization: Identifying the small percentage of patients who require immediate life-saving intervention and ensuring that resources are directed where they can have the greatest impact.
Nevertheless, certain challenges persist, she added. Hospitals must still address gaps in staff response rates during emergency activation, inconsistencies in documentation under pressure and the logistical complexities created by the arrival of family members with injured patients. These issues, she noted, are not unique to a single institution but reflect complications faced by healthcare systems across the region.
Moderated by Clinical Assistant Professor Elsy Jabbour, the session concluded with a reminder that preparedness is not a static protocol but an evolving process. Emergency plans must be continuously tested, revised and reinforced through training and simulation, particularly in environments where uncertainty is the norm.
Continuing Medical Education (CME) and Continuing Professional Development (CPD) credits were granted by LAU’s CME/ CPD Office to medical professionals who attended.
