First Pulsed-Field Ablation in Lebanon Takes Place at the LAU Medical Center
Dr. Johny Abboud uses the latest ablation technology to treat cardiac arrhythmias, making the center the first nationwide to perform this innovative procedure.
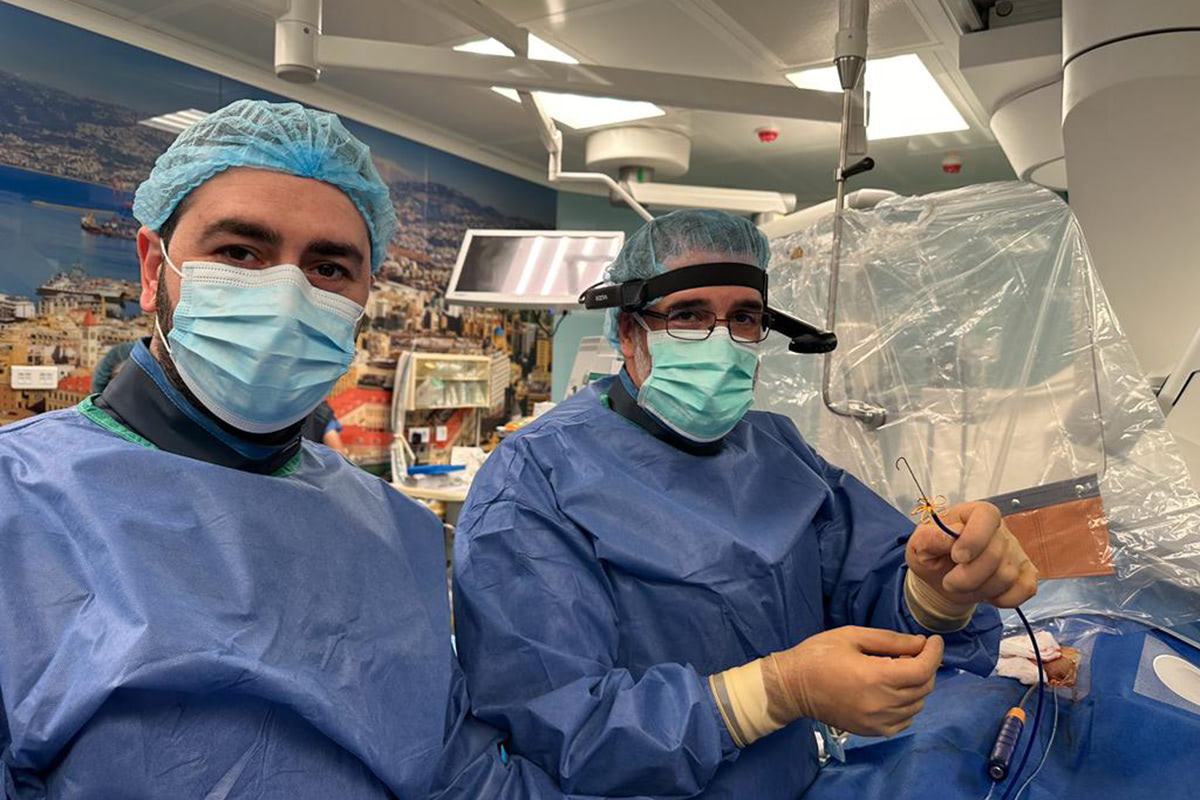
A team from the cardiac arrhythmia unit at the LAU Medical Center–Rizk Hospital performed a new procedure on 22 January 2024, the first in Lebanon, to treat a patient suffering from irregular heartbeats in the atria—the heart’s upper chambers—known as atrial fibrillation.
The pulsed-field ablation procedure was conducted under the supervision of Dr. Johny Abboud, clinical assistant professor and program director of the cardiology fellowship at LAU’s Gilbert and Rose-Marie Chagoury School of Medicine. The pulsed-field ablation (PFA) system by Boston Scientific—which received FDA approval as recently as January 2024—relies on electric pulses, a safer and more effective form of energy, to treat this condition.
“Every capable center will eventually switch to this technology,” said Dr. Abboud, “and we, in collaboration with Dr. Rony Al Nawar from the anesthesia team, Dr. Julie Ferzli from the radiology team and Dr. Richard Zalloum from the cardiology team, among other OR team members, are lucky to be the first to do so in Lebanon.”
Atrial Fibrillation is the most common arrhythmia, estimated to affect 33 million people worldwide and accounts for significant morbidity and mortality. The overall lifetime incidence increased to around 30 percent due to the aging of the population and lifestyle changes. Uncontrolled hypertension, obesity, sleep apnea, diabetes, thyroid dysfunction and many other conditions are associated with atrial fibrillation.
The risk of stroke in atrial fibrillation is secondary to blood clot migration from the heart to the brain. It ranges between 1 and 20 percent per year depending on other comorbidities.
Besides medication like blood thinners, and anti-arrhythmic and heart rate drugs, ablation—a minimally invasive surgical procedure that involves blocking electrical pathways in the heart using a catheter—has become the preferred treatment for many patients.
Conventional cardiac ablation, which relies on thermal energy to heat or freeze tissues in the heart and block its faulty electrical signals, has been in practice for the past 40 years. But the treatment comes with its own set of complications and can cause “phrenic nerve palsy, perforation, fatal bleeding, and narrowing of the pulmonary veins,” explained Dr. Abboud.
The safer PFA system, on the other hand, uses non-thermal energy to selectively disrupt myocardial cells function and block electrical conduction through these cells.
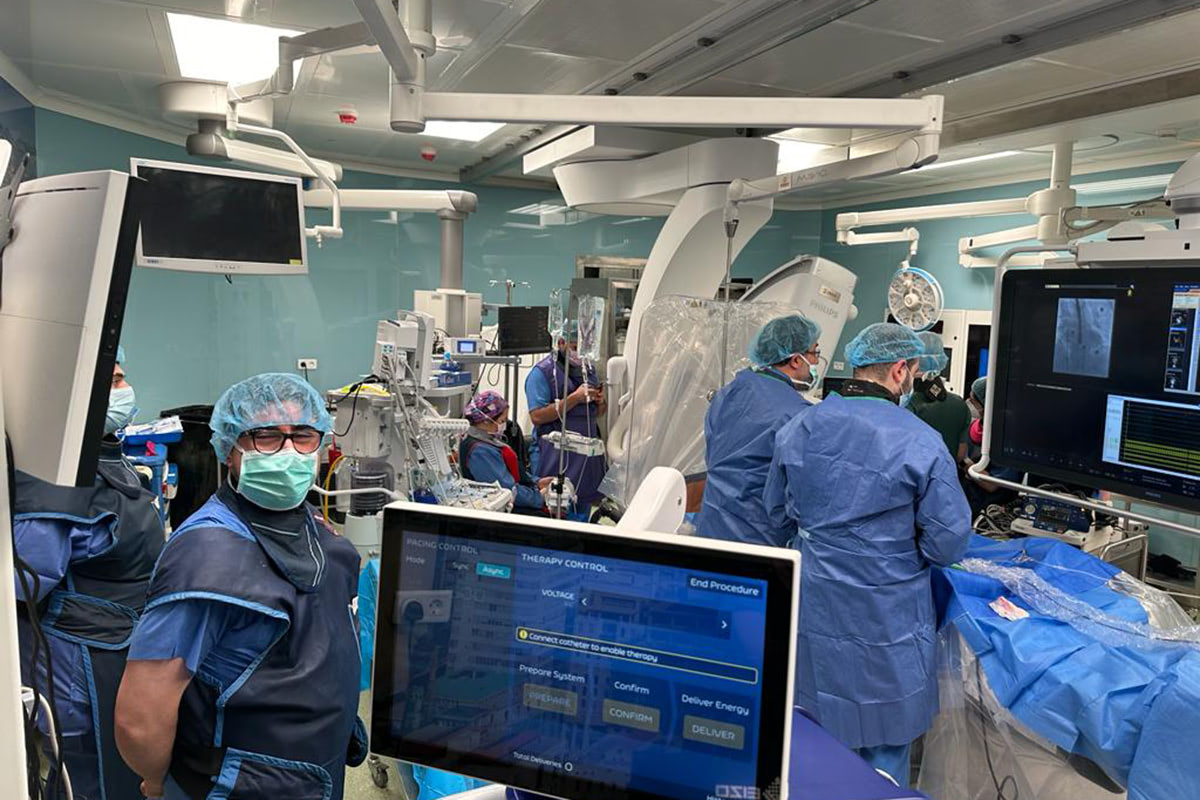
The procedure needs special training and a multidisciplinary approach from the cardiology, cardiothoracic, anesthesia and radiology teams. The cutting-edge technology used during this procedure demands a lot of expertise and is always assisted by the engineers from the Boston Scientific Company.
Although he had completed his training on the technology with Boston Scientific last year, Dr. Abboud had to wait for the equipment to arrive in Lebanon to carry out the procedure.
He opted to conduct the procedure, which was followed by another two cases, in the hybrid operating room at the LAU Medical Center–Rizk Hospital, which is already equipped with a state-of-the-art 3D mapping system thanks to a grant from the United States Agency for International Development’s (USAID) American Schools and Hospitals Abroad (ASHA). USAID administers the US foreign assistance program providing economic and humanitarian assistance in more than 80 countries worldwide.
The integration of the pulsed field ablation catheters in the Rhythmia HDx 3D mapping system will open new potentials in the near future for ablating not only atrial fibrillation but also all kinds of cardiac arrhythmias.
The PFA procedure, which was approved by the Conformité Européenne well before the FDA, has seen fewer than 1 percent complications in 40,000 cases, circumventing all major complications associated with conventional ablation methods, said Dr. Abboud.
Because of the proven safety and efficacy of the technology for treating AFib, especially in its earliest stages, this transformative treatment should be brought to the attention of the wider community, general physicians and cardiologists, he concluded.
“Our commitment to advancing healthcare goes beyond treating conditions—it is about revolutionizing the patient experience and setting new frontiers in medical education,” commented Dr. Sola Aoun Bahous, dean of the Gilbert and Rose-Marie Chagoury School of Medicine. “In the rhythm of these advancements, we find our true calling: shaping the future of medicine, one heartbeat at a time,” she added.
This is not the first time the cardiology department at the LAU Medical Center–Rizk Hospital has grabbed headlines for its pioneering use of the latest technology and expertise to enhance patient care. Back in 2015, Dr. Georges Ghanem, clinical professor at the school of medicine and head of the cardiology division, made history as the first cardiologist in Lebanon to perform a MitraClip procedure, to fix the mitral valve, without resorting to open-heart surgery. Similarly, in 2012, Dr. Ghanem and his team at the LAU Medical Center–Rizk Hospital launched the first Transcatheter Aortic Valve Implantation (TAVI) program in the country.